 Patients aged 18 and older with primary invasive breast cancer Denominator Criteria (Eligible Cases): For more information regarding Application Programming Interface (API), please refer to the Quality Payment Program (QPP) website. The quality data codes listed do not need to be submitted by MIPS eligible clinicians, groups, or third party intermediaries that utilize this modality for submissions however, these codes may be submitted for those third party intermediaries that utilize Medicare Part B claims data. The numerator options included in this specification are used to submit the quality actions as allowed by the measure. The listed denominator criteria are used to identify the intended patient population. Measure data may be submitted by individual MIPS eligible clinicians, groups, or third party intermediaries. This measure may be submitted by Merit-based Incentive Payment System (MIPS) eligible clinicians who perform the quality actions described in the measure based on the services provided and the measure-specific denominator coding. This measure is to be submitted each time a procedure is performed during the performance period for patients age 18 years and older who are operated upon for invasive breast cancer that are clinically node negative (clinical stage T1N0M0 or T2N0M0) before or after neoadjuvant systemic therapy. The risk of lymphedema with a sentinel lymph node biopsy is universal.The percentage of clinically node negative (clinical stage T1N0M0 or T2N0M0) breast cancer patients before or after neoadjuvant systemic therapy, who undergo a sentinel lymph node (SLN) procedure. The most serious side effect is swelling in the arm, known as lymphedema. Infection is uncommon and can develop up to seven days later. Swelling or fluid builds up under the incision and can remain for several weeks. Lymph node biopsy surgery always produces some discomfort for about a week after the operation. Blue nodes, or "hot" nodes (nodes with high radioactive counts), are removed and called sentinel nodes. One or more sentinel lymph nodes are removed and looked at under a microscope. Blue-stained lymphatic channels are identified and followed to the sentinel node or nodes.Ĥ. A small cut is made in the armpit to search for the sentinel node or nodes. The lymphatic channels then absorb the dye.ģ. During the operation, the patient is injected with a blue dye around the nipple or breast cancer site.Ģ. No negative reactions have been reported when using this method.ġ. The radiation in the injection is no more than what is produced by chest X-rays or mammograms. 
The doctor uses a radiation detector during surgery to pinpoint the lymph node that has the highest radiation counts. This flows toward the lymph nodes and allows an X-ray image of the lymph nodes.ģ. A special substance with a small amount of radioactivity is injected where the tumor is.Ģ. The doctor will inject the radioactive material before surgery (preoperative) and the blue dye during surgery (intraoperative).ġ. This is called lymphoscintigraphy, or sentinel lymph node mapping. This will make it easier for the doctor to find the node. These will identify the first lymph node. To find the node, a special blue dye or radioactive substance is injected. A specialist will look at the node to see if there are any cancer cells. Only the first lymph node in a group is removed during the biopsy. Removing the nodes from the areas is known as axillary lymph node dissection. If cancer cells are present in the first node, the lymph nodes in the affected area may require removal. If no cancer is found in the first node, the cancer has probably not spread to other nodes in the area. 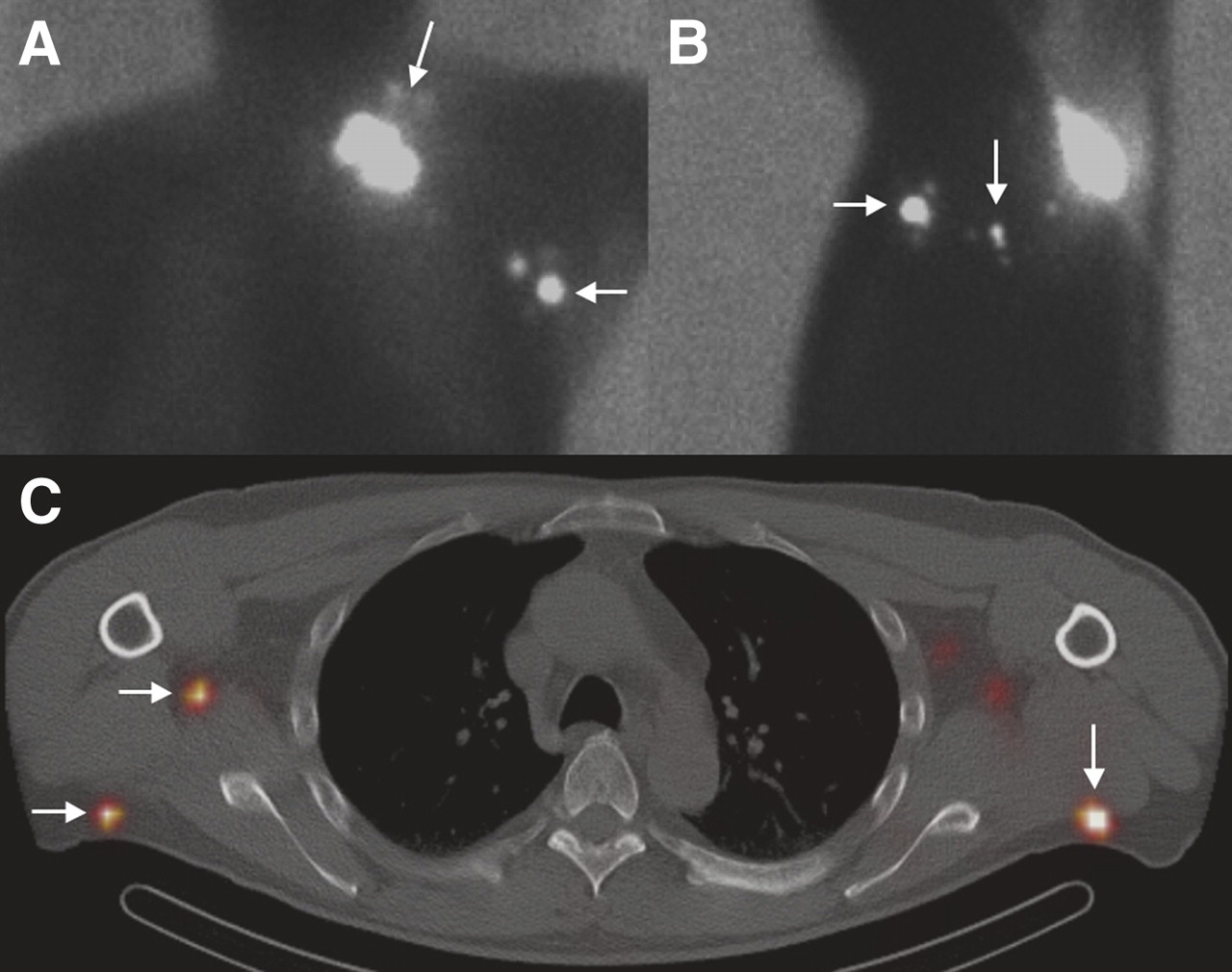
The first node in the group is known as a sentinel node. Breast cancer can spread to the nearby tissue in the underarms (axillary). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
